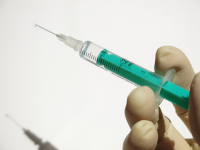
Osteoarthritis is a difficult problem to treat. The most definitive solution is of course replacing part or all of the knee. Many of our patients are looking for nonoperative options for their pain related to osteoarthritis prior to undergoing an extensive surgery. The good news is that one more option has become...
-
Knee Osteoarthritis Update- A New Injectable Option
-
What is Body Mass Index (BMI)?
Body mass index (BMI) is used in healthcare as a measurement of body fat and as a health predictor. Calculated by weight/height2, it is easy to find yours on an app or website. We have to include every patients BMI in their charts for insurance billing as well as anesthesia clearance for our surgical patients. But are we...
-
GIRD-Not Just For the Pros
At least once a week I have a conversation with a young up and coming baseball or softball player about GIRD (Glenohumeral Internal Rotation Deficit). This diagnosis is not just for pitchers; honestly it is really not limited to throwers as we see it in many overhead athletes. So what the heck is it? GIRD is...
-
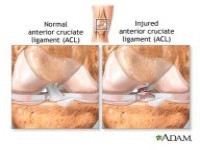
ACL Rehab Why Does It Take So Long to Heal?
We perform close to 100 ACL reconstructions a year here at the Grossteam. Our patient population can vary from weekend warriors to high level collegiate athletes and everyone in between. However, no matter what level of sport or career a patient is trying to get back to I find myself answering similar...
-
Spring Training-Pitch Counts Matter!
With warm weather comes baseball and softball spring workouts. We see a lot of players getting ready for both high school and club teams in our practice and there are a few pitfalls I would like to help players avoid. Pitch Counts Matter!!!! Did everyone hear me? I know you are big and strong and can...
-
Ortho Gadgets-What do I do with all this stuff?
We live in a technology driven world and orthopedics is no different. We have a device for just about everything. When you come in for an appointment you may be stressed about an injury, your insurance, or the upcoming surgery and what each device does may be clouded. Let's go over a few of the...
-
How To Have The Perfect Appointment
Have you ever walked out of the doctor’s office feeling disappointed, confused, wanting more? You had questions left to ask, things to discuss, you do not even know exactly what went on? I never want that to happen to you again! I think together we can help you have the PERFECT appointment. All appointments must start...
-
Youth Safety Month
It is Spring! This time of year brings warmer temperatures, longer days, outdoor activities and spring sports! Many youth athletes are changing out their basketballs, wrestling uniforms and hockey sticks for running shoes, baseball gloves and bicycles. Youth sports is a fantastic opportunity for kids. Athletes learn about teamwork and physical fitness. However, with sport comes risk. According to...
-
ACL Tears-That Terrible Pop You Felt in Your Knee
We hear it all the time, "I felt this pop in my knee." It may occur skiing, playing basketball, soccer, or even while at work. Rest assured that when you feel it, you will know something happened in your knee. The "pop" sensation is often followed by swelling, instability, and a trip to see me!
-
Happy National PA Week!!
Every year from October 6th-12th is national Physician Assistant week. Since you are my friends, family, and patients, I thought it only fair to celebrate with you! Several times a year I get asked questions about if I like my job, what I do, and how long I went to school, etc. This is a...